Ever wondered why your doctor or pharmacist suggests a generic version of a medication? You might worry if a cheaper pill actually does the same thing as the expensive brand-name version. The short answer is yes, but that "yes" is backed by a mountain of data and strict government oversight. In the US, the FDA is the federal agency responsible for protecting public health by ensuring the safety, efficacy, and security of human and veterinary drugs. They don't just take a manufacturer's word for it; they demand proof that a generic is a mirror image of the original in terms of performance.
When you pick up a generic, you're benefiting from a system designed to lower costs without compromising your health. In fact, generics now account for over 90% of all prescriptions filled in the US. But how do we know they're actually the same? It comes down to two main concepts: pharmaceutical equivalence and bioequivalence.
The Gold Standard: Pharmaceutical Equivalence
Before a drug even gets to the testing phase in humans, it has to be pharmaceutically equivalent. This means the generic must be a carbon copy of the brand-name drug in several key areas. To meet these generic drug quality standards, the medication must have the exact same active ingredient, strength, dosage form (like a tablet or a capsule), and route of administration (like oral or injection).
Now, if you've ever noticed that your generic pill is a different color or shape than the brand name, don't panic. The FDA allows differences in "inactive ingredients." These are things like fillers, binders, or dyes that don't affect how the drug works in your body. While the active chemical must be identical, the generic might use a different coloring agent or a different type of starch as a binder. As long as these additives don't interfere with the drug's performance, they're perfectly fine.
Proving Performance: What is Bioequivalence?
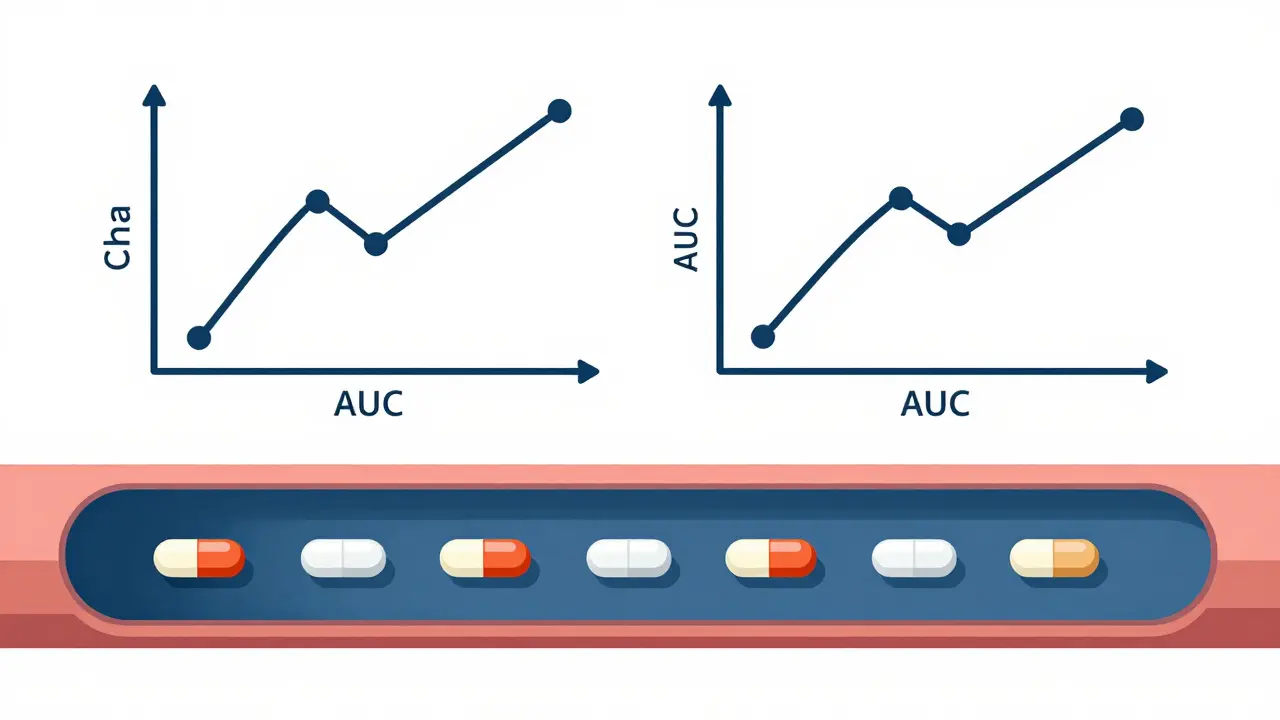
Being chemically the same is one thing, but the drug also has to behave the same way once it hits your bloodstream. This is where Bioequivalence comes in. Bioequivalence is the scientific proof that the generic drug delivers the same amount of active ingredient into the bloodstream at the same rate as the brand-name drug.
The FDA uses a very specific math formula to verify this. They look at two main metrics: Cmax (the maximum concentration of the drug in the blood) and AUC (the area under the curve, which represents the total drug exposure over time). For a generic to be approved, the 90% confidence interval for the ratio of these means must fall between 80% and 125%. If the drug absorbs too slowly or too quickly, it fails the test. Most small-molecule generics prove this through studies involving 24 to 36 healthy volunteers, ensuring the drug's behavior is consistent across different people.
| Feature | Pharmaceutical Equivalence | Bioequivalence |
|---|---|---|
| Focus | Chemical composition and form | Rate and extent of absorption |
| Requirement | Identical active ingredient and strength | Blood concentration levels (Cmax/AUC) |
| Allowed Variation | Inactive ingredients, color, shape | 80% to 125% acceptance range |
| Goal | Physical sameness | Therapeutic performance |
The Path to Approval: The ANDA Process
A company doesn't just start selling a generic drug; they have to submit an Abbreviated New Drug Application, or ANDA. It's called "abbreviated" because the generic company doesn't have to repeat the massive, multi-year clinical trials that the original brand-name company did to prove the drug works. Instead, they only need to prove that their version is the same as the already-approved brand.
The ANDA process is rigorous. It involves multiple review cycles where the FDA's Office of Generic Drugs scrutinizes the chemistry, manufacturing, and controls. They also demand stability testing. Manufacturers must prove the drug stays potent over time, often by putting it through "accelerated stability studies"-basically stressing the drug at 40°C and 75% humidity for six months to simulate long-term storage. If the drug breaks down too quickly, it won't get the green light.
Manufacturing Standards: cGMP
Quality doesn't stop at the lab; it extends to the factory floor. All drug manufacturers must follow current Good Manufacturing Practices, known as cGMP. These are codified in 21 CFR Parts 210 and 211. These rules ensure that every single batch of medicine is made the same way every time.
Under cGMP, everything is tracked. From the moment raw materials arrive at the warehouse to the moment the final pill is boxed, there's a paper trail. The FDA conducts about 3,500 inspections annually worldwide to make sure these facilities aren't cutting corners. An interesting fact is that about 50% of generic drugs are actually made by the same brand-name companies that invented them, often using the exact same machines and facilities.
The Challenge of Complex Generics
Not all drugs are easy to copy. While a simple tablet is straightforward, things like inhalers, topical creams, or long-acting injectables are "complex generics." For these, a simple blood test isn't enough to prove they work. A cream needs to penetrate the skin in a specific way, and an inhaler needs to deliver a precise mist to the lungs.
To handle this, the FDA has developed over 2,100 product-specific guidances. These act as a specialized playbook for manufacturers, requiring additional structural characterization tests to ensure "Q3 sameness." This means the physical and chemical properties are so close that the drug's delivery system functions exactly like the original. This is why some specialized medications take longer to reach the generic market than others.
Real-World Impact and Patient Experience
The result of these strict standards is a massive win for the wallet. In 2022 alone, generic drugs saved the U.S. healthcare system roughly $37 billion. Most people are happy with the switch; surveys show nearly 90% of adults are satisfied with their generics. However, it's not a perfect science for everyone.
For drugs with a "narrow therapeutic index"-where a tiny change in dose can be dangerous-some patients notice a difference. For example, some people switching between different generic versions of levothyroxine (for thyroid issues) have reported fluctuations in their levels. While the drugs are all within the 80-125% FDA range, that small variance can matter for certain highly sensitive conditions. This is why some doctors prefer you stay with one specific generic manufacturer once you've found one that works for you.
Are generic drugs as safe as brand-name drugs?
Yes. The FDA requires generic drugs to have the same active ingredients, strength, quality, and performance as the brand-name version. They must meet the same strict cGMP manufacturing standards and prove bioequivalence, meaning they work in the body in the same way.
Why are generics so much cheaper if they are the same quality?
Generic manufacturers don't have to pay for the initial research, development, and massive clinical trials that the brand-name company funded. Since they can use the original drug's safety and efficacy data via the ANDA process, their overhead is much lower, and they pass those savings to the consumer.
Can a generic drug have different inactive ingredients?
Yes. While the active pharmaceutical ingredient must be identical, the fillers, binders, and dyes (inactive ingredients) can differ. These do not affect how the drug treats the condition, though in very rare cases, a patient might have an allergy to a specific dye or filler used in a generic version.
What is the 80% to 125% rule in bioequivalence?
This is the FDA's standard for ensuring a generic drug's absorption is similar to the brand name. The 90% confidence interval for the ratio of the generic to the brand-name drug (for both peak concentration and total exposure) must fall within this range to be considered bioequivalent.
What happens if a generic drug doesn't meet these standards?
The FDA will issue a "complete response letter" informing the manufacturer that the application cannot be approved in its current form. The company must then fix the issues-whether it's a manufacturing flaw or a failed bioequivalence test-and resubmit the data for review.
Next Steps for Patients and Caregivers
If you're transitioning from a brand-name drug to a generic, the best approach is open communication. If you have a condition that requires very precise dosing (like epilepsy or thyroid disorders), tell your pharmacist you'd like to stick with the same generic manufacturer to avoid any minor fluctuations. If you notice a change in how you feel after a switch, don't stop the medication, but do contact your healthcare provider to discuss whether a different formulation is needed.
Comments (14)